There’s a particular kind of exhaustion that doesn’t show up on any blood test. Doctors rule things out one by one — thyroid, iron, vitamin deficiencies — and everything comes back normal. Meanwhile the person is falling asleep during the day, snapping at people they love, and quietly wondering if this is just what getting older feels like. For a significant portion of people in that situation, the answer is sitting in their airways, not their bloodwork. Sleep apnea treatment doesn’t just fix sleep. It resolves a chain of consequences most people never traced back to their breathing.
Not Just Loud Snoring
Sleep apnea gets dismissed so often because snoring feels like a minor complaint — embarrassing, maybe, but not exactly medical. What’s actually happening is far more disruptive. The airway collapses repeatedly through the night, oxygen drops, and the brain triggers a micro-arousal to restart breathing. The person never fully wakes, so they have no memory of it. What they have instead is a body that spent the night in low-grade physiological crisis, running stress responses that were never designed to operate for hours continuously.
Why Diagnosis Takes Years
Most people with sleep apnea spend years undiagnosed, and the reasons are genuinely worth understanding. The symptoms — fatigue, poor concentration, low mood, morning headaches — are non-specific enough to fit a dozen other conditions. GPs investigate the more obvious candidates first. Partners who mention the snoring get dismissed by the person themselves, who has no subjective experience of anything going wrong during sleep. There’s also a persistent demographic blind spot in clinical settings. Sleep apnea is strongly associated with older overweight men, which means women, younger adults, and those with normal body weight go unrecognised far longer than they should.
What It Does to the Heart
Every apnea event triggers a stress response. Blood pressure spikes, heart rate shifts, oxygen saturation drops. This doesn’t happen occasionally — it happens repeatedly across a single night, every night, for years before most people receive a diagnosis. Sleep apnea treatment interrupts that cycle entirely. Research consistently shows measurable reductions in blood pressure following effective treatment, even in people who had no idea their cardiovascular system was quietly under strain. The heart doesn’t announce the damage it’s accumulating. It absorbs it steadily until something forces the issue.
More Options Than Most People Know
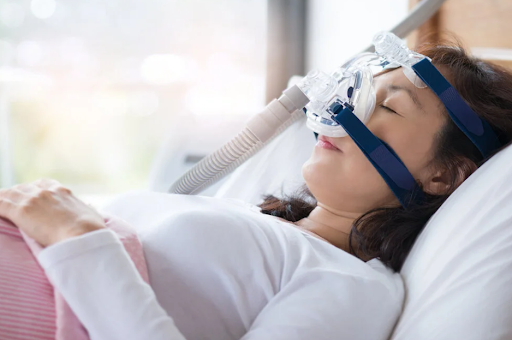
CPAP therapy has a real compliance problem, and most clinicians privately acknowledge it. The mask is uncomfortable, the machine bothers partners, and the psychological barrier of sleeping attached to equipment is genuine. What rarely gets communicated clearly enough is that CPAP is one option among several. Mandibular advancement devices reposition the jaw to maintain airway patency and suit milder cases well. Positional therapy works meaningfully for people whose apnea is position-dependent. Sleep apnea treatment that someone will actually use consistently is always preferable to the theoretically superior option they quietly abandon after a couple of weeks.
What Finally Pushes People to Act
It’s rarely fatigue alone that prompts someone to get assessed. More often it’s a relationship straining under disrupted sleep, a professional consequence from impaired concentration, or a GP who happens to ask the right questions. Sometimes it’s a close call while driving. The threshold differs for everyone, but the pattern stays consistent — people wait far longer than they should, and almost universally wish they hadn’t.
Understanding the Sleep Study
A sleep study measures how many times per hour breathing is disrupted across the night. Mild, moderate, and severe classifications shape treatment recommendations meaningfully. Home-based studies are accessible and adequate for most straightforward cases, though complex presentations warrant fuller in-lab monitoring. The result isn’t just a diagnosis — it’s the information that determines which treatment direction actually makes sense.
Conclusion
Sleep apnea treatment works, but the gap between when people should start it and when they actually do remains frustratingly wide. The condition mimics so many other things that years pass before anyone looks at the airway. What shifts after effective treatment isn’t just sleep quality — it’s the entire baseline of how someone functions and feels day to day. The tiredness that felt permanent lifts. The cardiovascular strain that was accumulating quietly reduces. Most people describe it as feeling like themselves again, which says everything about how thoroughly the condition had taken hold without ever being noticed.